All-On-X Dental Implants: One Secure Solution For A Full, Fixed Smile
When teeth are failing across the board, it’s not just one problem—it’s a daily burden. You may have trouble chewing, frequent breakage, repeated repairs, or gaps that keep growing. You might feel like you’re constantly “managing” your teeth instead of enjoying life. All-On-X dental implants were created for this exact situation: replacing a full arch of teeth with a secure, fixed solution supported by implants.
All-On-X dental implants don’t replace teeth one at a time. They rebuild an entire upper arch, lower arch, or both using a strategic number of implants. The result is a stable bridge of teeth that stays in place. For many patients, All-On-X dental implants feel like a reset—because daily comfort and confidence finally come back.
What All-On-X Dental Implants Mean And Why They’re Different
The “X” in All-On-X dental implants stands for the number of implants used to support the arch. Some people may need four, five, six, or another number depending on:
- Bone support
- Bite forces
- Jaw shape
- Your dentist’s plan for stability
The key point is this: All-On-X dental implants support a full row of teeth with a carefully planned implant foundation.
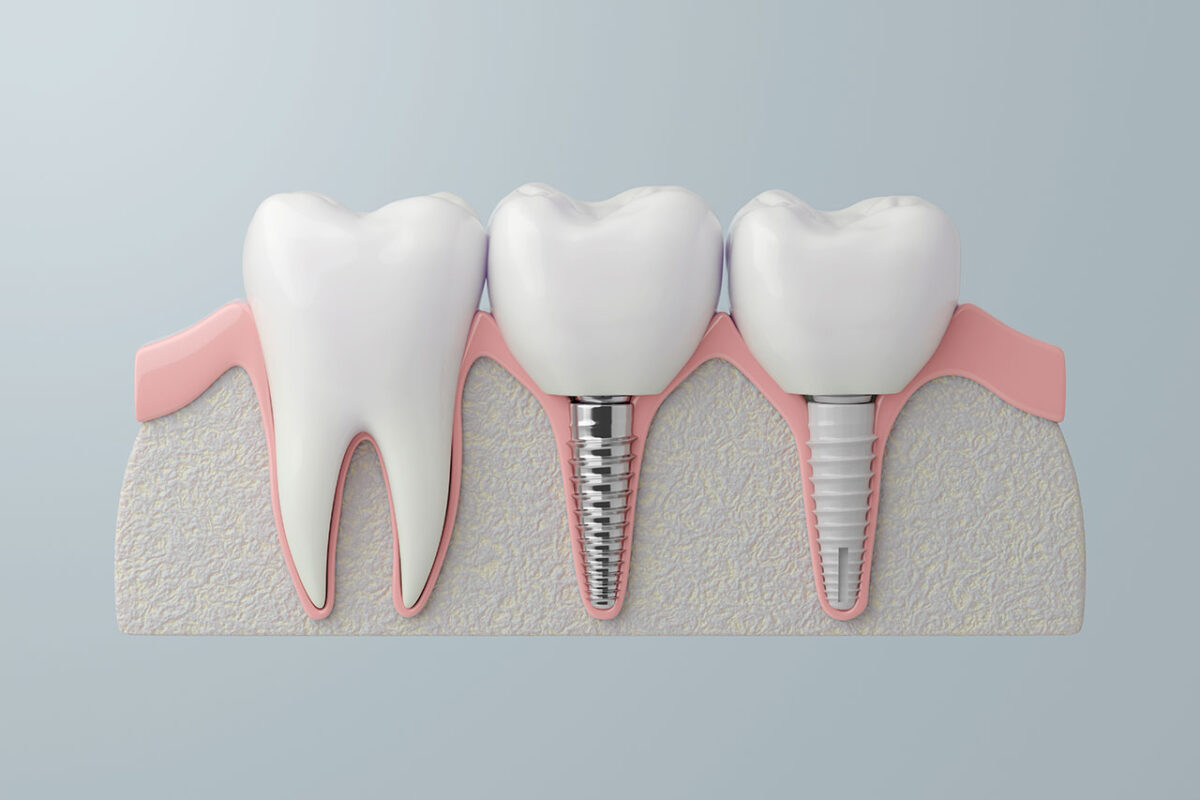
Instead of a removable denture resting on gums, All-On-X dental implants anchor a fixed bridge to implants. That anchoring changes how it feels to eat, talk, and live day to day.
Who All-On-X Dental Implants Are For
All-On-X dental implants may be worth exploring if you:
- Have many missing teeth
- Have teeth that keep breaking or need constant repair
- Have advanced wear, decay, or gum problems affecting many teeth
- Wear dentures but want a more stable solution
- Want a fixed smile that doesn’t come out at night
The best candidates for All-On-X dental implants are people who want a long-term solution and are ready for a step-by-step plan to rebuild their bite.
The All-On-X Dental Implants Process: What Happens First, Next, And Later
A big reason people delay treatment is uncertainty. The All-On-X dental implants process becomes much less intimidating when you see it as phases with a clear purpose.
Phase 1: Evaluation And Planning
Your dentist checks:
- Gum health and infection risk
- Bone support and anatomy
- Bite alignment
- Which teeth can be saved (if any) and which should be removed
Planning matters because All-On-X dental implants rely on implant placement that can handle strong chewing forces.
Phase 2: Preparing The Mouth
If there are teeth that can’t be saved, they may need to be removed. This step clears out pain sources and creates a healthier foundation. For many patients, removing failing teeth is a relief because the mouth stops being a constant problem.
Phase 3: Implant Placement
Implants are placed into the jawbone to act like secure anchors. In many cases, implants are positioned in areas of stronger bone to improve stability. This is one reason All-On-X dental implants can work well even for patients who have had tooth loss for a while.
Phase 4: A Fixed Set Of Teeth
Many All-On-X dental implants plans include a fixed temporary bridge during healing. Later, the final bridge is made for long-term strength and a natural look.
Your timeline depends on your mouth and healing needs. The important thing is that the plan is designed for safety and long-term performance.
Benefits Of All-On-X Dental Implants
All-On-X dental implants are often chosen because they combine full-arch replacement with strong stability. People want to eat, speak, and smile without fear of movement.
Benefits of All-On-X dental implants include:
A fixed smile that stays in place
All-On-X dental implants support a bridge that doesn’t rely on adhesives and typically doesn’t need to be removed daily.
Stronger chewing
Many patients find they can chew more confidently with All-On-X dental implants compared to removable dentures.
Improved day-to-day comfort
A stable bridge can mean fewer sore spots and less rubbing compared to options that rest on gums.
Support for jawbone
Because implants connect to bone, All-On-X dental implants can help provide stimulation that supports bone health over time.
A simplified full-arch plan
Instead of placing an implant for every missing tooth, All-On-X dental implants use a strategic number of implants to support the full arch.
Confidence in social moments
Patients often appreciate speaking and laughing without worrying about shifting or clicking.
All-On-X Dental Implants Vs. Traditional Dentures (No Tables—Just Real Differences)
Traditional dentures can help restore appearance and basic function, but they rest on gum tissue. Over time, the jawbone can shrink, and dentures can loosen. Some people do fine with dentures, while others struggle with movement, sore spots, and a limited diet.
All-On-X dental implants are anchored. That anchoring usually means:
- Less movement while chewing and speaking
- Less reliance on suction or adhesives
- A more “part of me” feeling for many patients
- More consistent function day to day
That doesn’t mean dentures are “bad.” It means All-On-X dental implants may fit better if you want a fixed solution and higher stability.
Caring For All-On-X Dental Implants
All-On-X dental implants are strong, but they still require daily cleaning and professional maintenance. The bridge may feel so secure that it’s easy to forget it needs consistent care—just like natural teeth.
Helpful habits include:
- Brushing daily along the gumline
- Using the cleaning tools your dental team recommends around the bridge
- Keeping regular professional cleanings and checkups
- Avoiding chewing ice or extremely hard items
- Wearing a nightguard if you grind your teeth
The goal is to keep gums healthy and keep plaque from building up around implant areas. This helps All-On-X dental implants stay stable long-term.
Common Concerns About All-On-X Dental Implants
“Will it look natural?”
A well-designed bridge is made to fit your face and smile shape. All-On-X dental implants can look very natural when planned properly.
“Is it a huge recovery?”
Healing varies, but many patients do better than expected—especially when they follow instructions closely. Your team will guide you on eating, cleaning, and comfort steps.
“What if I’m missing bone?”
Many people with bone loss can still be candidates for All-On-X dental implants because placement can be planned around stronger areas. An evaluation is the only way to know what’s best in your case.
All-On-X dental implants are designed for people who want a full-arch solution that stays in place, feels stable, and restores everyday function. They can help you move out of the cycle of broken teeth, repeated repairs, and worry about looseness. The best first step is a personalized exam to confirm candidacy and map out a plan that fits your goals and your health.
Ready to see if All-On-X dental implants are right for you? Contact Secure Dental to schedule your consultation or book an appointment at one of our convenient locations in East Peoria or Chicago, IL; Davenport, IA; or Hammond, IN—and take the next step toward a secure, confident smile.